Breast Cancer: Types, Symptoms, Diagnosis, Treatment - PMCC Denver Oncology
Breast cancer is a malignant disease in which the accelerated, disordered and uncontrolled proliferation of mammary gland cells forms a tumor that can invade neighboring tissues and distant organs of the body.
Breast cancer is the most common malignancy and is the most frequent cause of cancer death in women. In Europe and the United States, the mortality associated with breast cancer has decreased by 20-30% in the last 20 years, this is due to an increase in the detection of early-stage cancer due to the increasing use of mammography and the establishment of standardized detection systems; as well as improvement in treatment of localized breast cancer.
The possibility of cure and improvement in the quality of life of patients with breast cancer depends on the extent of the disease at the time of diagnosis and the proper application of all therapeutic resources.
Types of Breast Cancer
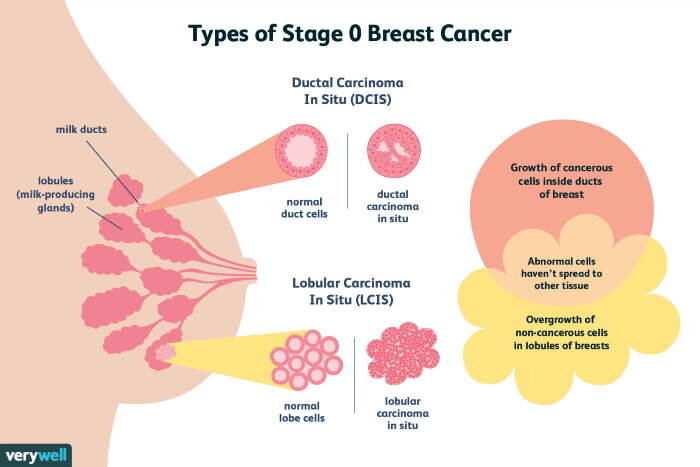
imagesource: verywellhealth.com
The histopathological classification of mammary carcinoma according to the World Health Organization (WHO) is divided into non-invasive (in situ), invasive and other (Paget's disease of the nipple).
Approximately 75-80% of cancers are invasive or infiltrating, this feature gives cells the ability to penetrate around the lymphatic and vascular channels causing metastasis. The most frequent histological type is the invasive ductal carcinoma that represents 70 to 80%, the second in frequency is the invasive lobular (5-10%), which is difficult to diagnose due to its diffuse dissemination. Other less common cancers are tubular, medullary, mucinous and papillary, among others.
Ductal carcinoma in situ (DCIS) remains confined to the ductal system of the breast without penetrating the basement membrane, approximately 30 to 50% of patients with DCIS develop invasive ductal carcinoma in a period of 10 years.
Lobular carcinoma in situ (LCIS) originates from the terminal ductal lobule and can be distributed diffusely through the breast. Women with LCIS are at an elevated risk of developing invasive breast cancer.
Paget's disease is relatively rare, accounting for approximately 1% of breast cancers, and it affects the nipple areola complex.
Have a Question About Breast Cancer? Contact Our Office.
Breast Cancer Risk Factors
There are certain factors that can act independently or together and promote the development of breast cancer. The presence of two or more risk factors increases the possibility of developing this disease. The most important risk factors are:
• Advanced age (> 55 years).
• Menstruation at an early age (before the age of 12).
• Old age at the time of first birth (34 years) or never having given birth.
• Personal history of breast cancer or benign (non-cancerous) breast disease (atypical ductal hyperplasia).
• Mother or sister with breast cancer.
• Treatment with radiotherapy directed to the breast/chest 10 to 15 years prior to the diagnosis of breast cancer.
• Breast density increased in a mammogram.
• Hormone replacement therapy.
• Consume alcoholic beverages.
• Caucasian races.
• Genetic alterations (BRCA 1 and BRCA 2 gene)
Symptoms of Breast Cancer
Most women with breast cancer have no signs or symptoms when the diagnosis is made. However, it is possible that patients present changes in the structure of the breast. The main symptoms are the following:
• Palpable nodule in the breast or armpit
• Spontaneous discharge through the nipple
• Nipple Retraction
• Irritation or redness of the breast
• Breast pain
Need Guidance with Breast Cancer? Explore Our Programs.
Breast Cancer Early Diagnosis
To establish the diagnosis of breast cancer, it is necessary to correlate clinical, radiological and histopathological findings.
General Recommendations
• Monthly breast self-examination from the age of 18 (seven days after the end of menstruation).
• Annual clinical breast examination after 25 years
• Annual screening mammography in asymptomatic women as of 40 years of age.
• Breast MRI or ultrasound is the initial choice study in women under 35 with breast disease.
Mammography
3D Mammography. Image by 3Dadept.com
Mammography is the imaging method of choice for the diagnosis of breast cancer, with a sensitivity of 70-90% for women over 50 years old, although approximately 10-15% of palpable cancers are not identified by this method. It is indicated to evaluate any abnormality detected by screening or by medical evaluation.
Ultrasound and MRI
In women under 50 years of age and pregnant women, breast ultrasound and MRI are indicated to evaluate abnormalities in the breast, it is also indicated to evaluate Mammography findings and as a guide for performing interventional procedures.
Biopsy
Fine needle aspiration biopsy has lower sensitivity and specificity than an excitional needle biopsy, so the latter is preferred since the tissue obtained maintains the tissue architecture and allows the distinction between invasive and non-invasive carcinoma. Biopsies performed with aspiration system obtain a greater number of calcifications, better characterization of complex lesions such as atypical ductal hyperplasia and DCIS and allow complete tissue excision.
It is important to remember that the definitive diagnosis of breast cancer is made based on the histopathological study of the tissue obtained by biopsy.
Clinical Stages
After having the histopathological diagnosis of cancer, laboratory studies should be conducted, aimed at determining the extent of the disease. The prognosis and treatment are individualized and will depend on the clinical stage of cancer, this is determined depending on the tumor size, the presence or absence of lymph node metastasis and/or distance. These stages, in a didactic way, are divided into early, locally advanced and metastatic disease.
Treatment
There are five main types of treatment for breast cancer. The use of these treatments will vary according to the clinical situation of each patient.
• Surgery
• Radiotherapy
• Chemotherapy
• Hormone therapy
• targeted therapy
Different factors condition the treatment plan, including the stage of cancer, the presence of hormonal receptors, the results of the gene expression profile, the general health of the patient, among others.
Local and Systemic Therapy
Local therapy is used to remove or destroy cancer directly where it is located. Surgery and radiation therapy are examples of local therapy.
Systemic therapy includes treatments that work throughout the body to attack cancer cells wherever they are. Chemotherapy, hormone therapy, and targeted therapy are examples of systemic therapy.
Adjuvant and Neoadjuvant Therapy
Neoadjuvant therapy is used before surgery to reduce the size of the tumor, which offers the possibility of choosing breast-conserving surgery instead of a radical mastectomy.
Adjuvant therapy refers to the treatment that is used after surgery to decrease the risk of cancer recurrence. Even when all cancer seems to have disappeared, doctors will sometimes recommend adjuvant therapy as an additional safety measure in case some cancer cells have escaped into the bloodstream. Adjuvant therapy reduces the risk of relapse.
Both neoadjuvant and adjuvant therapies for breast cancer may include chemotherapy, hormone therapy, targeted therapy and/or radiation therapy.
Breast-Conserving Surgery
Breast-conserving surgery involves removing the tumor along with a small edge of the healthy tissue. The goal of Breast-conserving surgery is to preserve as much breast as possible. During surgery for invasive cancer, one or more lymph nodes can also be removed to see if cancer has spread beyond the breast.
Mastectomy
Total mastectomy (also called simple mastectomy) removes the breast, including the nipple, but without removing the lymph nodes in the armpit.
Radical mastectomy removes the breast, including the nipple, some lymph nodes in the armpit and the pectoral muscle lining.
Radio-therapy
Radiation therapy is a local therapy that is used to destroy cancer cells that may have been left behind after surgery. It is almost always used after breast-conserving surgery to decrease the risk of cancer recurrence. It can also be used after a mastectomy if the tumor was larger than 5 cm or if the cancer invaded the lymph nodes
Chemotherapy
image source: verywellhealth.com
Chemotherapy is a type of systemic therapy that uses drugs to destroy or slow the growth of cancer cells anywhere in the body. Chemotherapy can be given orally or intravenously. It is usually administered at repeated intervals, for example, once a week or every two weeks. The treatment schedule of each woman varies depending on the drug or combination of specific drugs used.
The most common chemotherapy drugs used for the treatment of early stage breast cancer are the anthracyclines (such as doxorubicin or epirubicin) and taxanes (such as paclitaxel or docetaxel). These can be used in combination with other drugs such as fluorouracil, cyclophosphamide or carboplatin. Advanced breast cancer is treated more often with a single drug, although some combinations may also be used.
Hormone Therapy
Hormone therapy is a type of systemic therapy that works by blocking or decreasing the amount of hormones in the body. It is used only in patients whose breast cancer depends on hormones to grow (called breast cancer with hormone receptor positive). Hormone therapy is used more frequently after surgery to reduce the risk of cancer recurrence.
Tamoxifen is the most common hormone therapy to treat breast cancer with a positive hormone receptor. It works by blocking the effect of hormones on cancer cells.
Targeted Therapy
Targeted therapy is a systemic therapy that acts by blocking the action of specific substances contained in cancer cells, such as the HER2 protein which causes the growth and spread of cancer. The most commonly used drug is trastuzumab (Herceptin).
Sources
1. Early Breast Cancer Trialists’ Collaborative Group (EBCTCG). Effects of chemotherapy and hormonal therapy for early breast cancer on recurrence and 15-year survival: an overview of the randomised trials. Lancet 2005;365:1687-717.
2. Destouet JM, Bassett LW, Yaffe MJ, et al. The ACR’s mammography accreditation program: ten years experience since MQSA. J Am Coll Radiol 2005;2:585-948.
3. Goss PE, Ingle JN, Ales-Martinez JE, et al. Exemestane for breast-cancer prevention in postmenopausal women. N Engl J Med 2011;364:2381-91.
4. Goldstein NS, Murphy T. Intraductal carcinoma associated with invasive carcinoma of the breast. A comparison of the two lesions with implications for intraductal carcinoma classification systems. Am J Clin Pathol 1996;312-316
5. Toth BA, Lappert P. Modified skin incisions for mastectomy: the need for plastic surgical input in preoperative planning. Plast Reconstr Surg 1991;87:1048.